The first artificial kidney built in Canada has ties to London: A revolution in care for patients with kidney failure

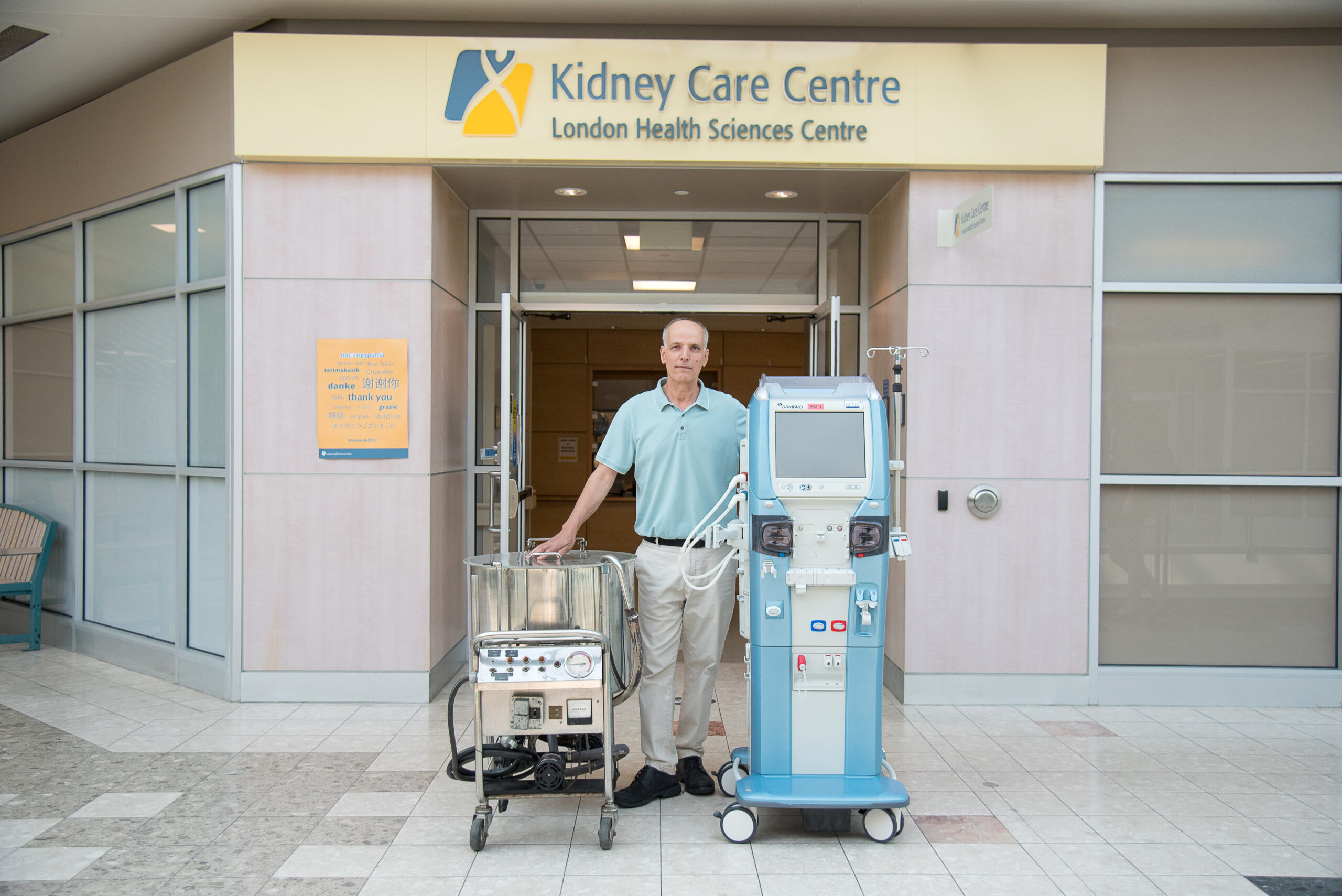
Above: Sal Treesh, Charge Technologist, Regional Renal Program with a second generation of the Kolff machine in LHSC’s Kidney Care Centre (left) and a current hemodialysis machine (right)
Many firsts and innovations have occurred at London Health Sciences Centre (LHSC) over the past 150 years, and that extends into renal care where a life-changing machine called the “Kolff kidney” was built in Canada for the first time right here in London.
The first artificial kidney was invented by Dr. W.J. Kolff, head of the medical department in Kampen, the Netherlands during World War II. The first one built in Canada was by J. Van Noordwijk, a Dutch scientist working in London under a research grant from Western University and was a combined effort between the Departments of Physiology Clinical Pathology at LHSC and, the Faculty of Medicine.
Referred to as the “Kolff kidney” after its inventor, a second generation of the device is still in London in one of the waiting areas in LHSC’s Kidney Care Centre. It is kept in a protective display case so patients, staff and visitors to the centre can appreciate how far kidney care has come in the past 76 years.

How it works
The first artificial kidney mimicked the kidney’s natural functions to filter blood and maintain fluid balance – like what today’s hemodialysis machines do for patients in kidney failure.

The old device was run by an electric motor and was made of around 20 metres of cellophane tubing wrapped around a rotating drum. The drum rotated in a salt solution. The patient’s blood entered one end of the tube, went through the cellophane casing and became immersed in the saline solution where impurities in the blood passed through the pores of the cellophane into the solution. The blood would be purified at the other end.


Sal Treesh, Charge Technologist, in LHSC’s Regional Renal Program notes, “The invention of the artificial kidney “dialyzers” has resulted in many lives saved around the world. Without dialysis and kidney transplantation, end stage renal failure meant the termination of a patient’s life in the past. The Kolff kidney has opened the door for new innovations and developments to improve the quality of human life.”
Treesh also comments on how far this technology has come in such a short time. “The hemodialysis machines we have now act similarly to the old machine but are far more advanced and efficient. What used to take 20 metres of cellophane tubing to filter the blood, today’s dialyzers consist of thousands of tiny, hair-thin, semipermeable hollow fibers bundled together within a cylindrical plastic casing of about 6 to 12 inches long with different types of membranes to suite patient’s needs and facilitate more efficient removal of waste products and toxins during dialysis.”
The white tube on the side of the machine performs the same function as what the entire tank accomplished in the “Kolff kidney.”

Today’s hemodialysis machines provide more control over the treatment strategy for each patient. They also provide:
- More automation with higher efficiency.
- Very efficient disinfection processes with automatic start and stop functions.
- High-quality fluid – eliminating the need for saline bags.
- Increased patient well-being and a reduced need for nurse intervention.
- Real-time monitoring and consistent reaches of the prescribed treatment dose.
- Data collection of fluid prescribed for the treatment and the fluid removed from the patient. This data is analyzed in real time to display up to date values of clearance measurement and patient’s blood volume to allow clinicians to alter treatment parameters if needed so they consistently reach the prescribed dose.
- Some advanced features that may improve the quality of dialysis:
- Hemocontrol: This function utilizes continuous monitoring of dialysis parameters to optimize blood purification efficiency and minimize the risk of complications.
- Hemodiafiltration (HDF): This function is used to remove larger molecules and toxins from the blood which are not effectively cleared by standard hemodialysis alone.
“It is exciting to see how this technology has changed over the decades to support renal patients and continues to improve with ongoing research and treatment developments,” says Treesh.
LHSC is celebrating 150 years of care, innovation, and community impact by sharing 150 moments from our history. Join us in marking this milestone by sharing your own LHSC story.
link